Reading time: 15 min
Summary of: A Complete Guide to Disc Degeneration for Quebec Patients
Ce guide complet aborde la dégénérescence discale, un processus d'usure des disques intervertébraux, ses causes, symptômes, diagnostics et traitements. Destiné aux patients québécois, il présente des options de traitement conservateur, y compris la décompression neurovertébrale, et compare les approches québécoises et françaises en matière de soins. Les témoignages de patients illustrent les parcours de soins et les résultats possibles.
Top 5 Things to remember
- La dégénérescence discale est un phénomène naturel lié au vieillissement.
- Les traitements conservateurs, comme la physiothérapie, sont souvent efficaces avant d'envisager la chirurgie.
- La décompression neurovertébrale est une option non chirurgicale innovante pour soulager les douleurs discales.
- Les témoignages de patients montrent que de nombreuses personnes peuvent éviter la chirurgie grâce à des traitements appropriés.
- Il existe des différences significatives entre les approches de traitement au Québec et en France.
Listen to our Podcast
This podcast explores disc degeneration, a progressive wear and tear of the spinal discs, explaining its causes, symptoms and diagnosis. Conservative treatments, such as decompression, are discussed. […]
A Complete Guide to Disc Degeneration for Quebec Patients
There disc degeneration (or degenerative disc disease) refers to the process progressive wear and tear of the intervertebral discs located between the vertebrae of the spinal column. These discs, which are normally elastic and hydrated, act as shock absorbers between the vertebrae. Over time, they deteriorate, losing flexibility and height, and becoming less effective shock absorbers. This wear and tear sets in slowly, and can affect any part of the spine (neck, back or lower back). When it becomes symptomatic, we speak of degenerative disc disease. It's a phenomenon generally linked to natural aging, although it can be accelerated by other factors. In this guide, we will explain in a clear and reassuring way what disc degeneration is, how it occurs and how to prevent it. causes and symptoms, We'll look at how it's diagnosed, and what treatments are available. In particular, we will present conservative treatment options (such as physiotherapy, exercises, medication or non-invasive decompression), treatments to be preferred before surgery, and in particular the neurovertebral decompression offered by TAGMED. Finally, we'll look at situations requiring surgery, including solutions offered in France at referral centers, and compare the Quebec approach with the French one. From patient testimonials and real-life examples to help you better understand and plan your care pathway.
1. Understanding disc degeneration
Definition and process
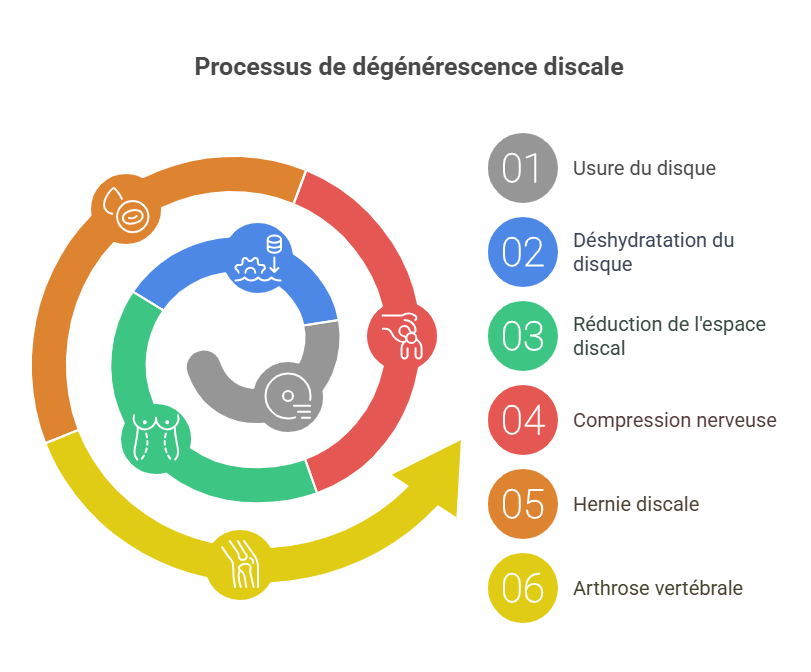
An intervertebral disc is a cartilaginous cushion between two vertebrae, composed of a gelatinous center (nucleus pulposus) and a fibrous ring. With age and repeated stress (carrying loads, repetitive movements, accidents), discs are subject to wear progressive. We speak of disc degeneration when one or more discs deteriorate abnormally and become less effective in their shock-absorbing role. Specifically, the disc tends to dehydrate (lose water), making it stiffer and thinner. As a result, it is less able to withstand the pressures and movements of the spine, and the vertebrae move closer together. This reduction in space can also reduce the passage of spinal nerves through the foramens (intervertebral openings). Degeneration disc is therefore often linked to natural aging, but when wear and tear leads to severe pain or loss of mobility, it becomes a real pathology that needs to be treated.
In most cases, disc degeneration sets in slowly. At first, it may go unnoticed or cause only mild discomfort. Over time, however, disc damage can lead to complications such as the appearance of’herniated discs or’spinal arthrosis (also known as discarthrosis). A herniated disc occurs when the cracked annulus fibrosus allows part of the nucleus pulposus to escape outside the disc - often towards the spinal canal - which can compress adjacent nerve structures. The presence of significant degenerative disc disease at a vertebral level thus increases the risk of risk of slipped disc at this level. In short, degeneration disc is a phenomenon of’wear of discs, which reduces their mechanical efficiency and can indirectly cause pain and other problems if nerves are irritated or spinal stability is diminished.
Here is a structured list of the main French synonyms for «disc degeneration», with their nuances:
Typical symptoms
The main clinical sign of degenerative disc disease is the backache. The precise location of the pain depends on the area of the spine affected. A general distinction is made between :
- Lumbar disc disease (lower back) - It causes back pain that can radiate to the buttocks or legs. Chronic low-back pain may be accompanied by stiffness and difficulty in performing certain movements (bending, lifting, etc.). If a herniated lumbar disc is associated, a pain of the sciatica may occur (pain moving down the leg, numbness, tingling).
- Back disc disease (middle of the back) - More rare, it is characterized by back pain (pain between the shoulder blades) or high back). Back pain of disc origin can sometimes interfere with breathing or rotation of the torso. It is less frequent because the thoracic spine is more rigid (supported by the rib cage).
- Cervical disc disease (neck) - Neck pain can radiate to the shoulders, shoulder blades and arms. Neurological symptoms such as numbness, tingling in the hands or weakness in one arm can occur if the cervical nerves are irritated or compressed. In severe cases, cervical disc disease can even cause manual dexterity or balance problems (signs of spinal cord compression if the spinal cord is affected).
In addition to the pain, the stiffness of the spine is a frequent symptom. Many patients experience a loss of flexibility and discomfort in performing certain daily activities (e.g. difficulty in bending over to tie shoes in the case of chronic low-back pain). Pain is often mechanics They are aggravated by activity or certain positions, and relieved by rest. However, during acute phases (attacks), pain can be severe even at rest, severely limiting activity.
It's important to note that disc degeneration evolves in flare-ups. Painful episodes can last from a few weeks to a few months, interspersed with phases of relative calm. Over time, seizures may become more frequent Some patients experience chronic pain. For these patients, the impact on quality of life can be major: sleep disturbance, difficulty in working, driving or enjoying leisure activities, etc. The chronic pain associated with degenerative disc disease can even lead to anxiety or depression if left untreated. care adequately. That's why it's so important to seek advice and intervene before you reach such extremes.
Causes and risk factors
The main factor in disc degeneration is the aging. Inevitably, with age, intervertebral discs undergo a progressive drying out of the gelatinous core and a stiffening of the annulus fibrosus. By the age of forty, a certain degree of disc wear is common even in people with no symptoms. However, several factors can accelerate or aggravate this natural wear and tear:
- Genetic predisposition : some people have a less resistant disc structure from birth, or a family history of early disc disease.
- Trauma and repetitive strain injuries : accidents (falls, car accidents) or years of intense physical work can damage discs more quickly. Repeated incorrect movements (poor work postures, lifting without back protection) create cumulative micro-injuries.
- Overweight and obesity: excess weight increases pressure on the discs, particularly those in the lower back, accelerating their deterioration.
- Sedentary lifestyle : lack of physical exercise weakens the muscles that support the spine (abdominal, paravertebral). A poorly supported spine more stress on the discs. Paradoxically, regular moderate exercise helps to preserve discs by strengthening the musculature and maintaining good cartilage hydration.
- Poor lifestyle habits: smoking is known to reduce disc vascularization and promote dehydration. A poor diet can also play a role (for example, a lack of nutrients or an excessively acidic diet could contribute to inflammation and disc degeneration).
- Pre-existing pathologies : spinal problems such as recurrent herniated discs, some forms of arthritis or osteoarthritis, or a history of back surgery (e.g. after nucleolysis or disc surgery) can accelerate wear on an adjacent disc.
It is often difficult to identify a single cause of disc degeneration. It's usually a combination of factors (age + genetics + lifestyle) that gradually leads to wear and tear. Every patient is different: some will present significant signs of disc disease at 30, while others will have discs in relatively good condition at 60. Whatever the case, a good health practices (regular physical activity, protecting the back when exerting oneself, maintaining a healthy weight, avoiding smoking) can slow the progression of disc wear or mitigate its consequences.
Diagnosis
The diagnosis of disc degeneration begins with a clinical examination complete. The physician (often a family doctor, a physiotherapist, a medical rheumatologist or an orthopedist) will examine your back and neck, test spinal mobility, look for sore spots and assess the condition of the paravertebral muscles. He or she will also check for signs of neurological These include numbness, muscle weakness and reduced reflexes, which could indicate that a nerve is compressed by a degenerative disc or herniation. This clinical examination already helps to orient the diagnosis and rule out other causes of back pain (such as a muscular or joint disorder, or another pathology).
To confirm the diagnosis and assess the extent of the lesions, we use examinations of’medical imaging are generally required. The standard spinal X-ray may show a pinched disc (narrowing of the space between two vertebrae), osteophytes (parrot beaks caused by osteoarthritis) or other signs of wear and tear. However, the most useful examination is the’MRI (magnetic resonance imaging). MRI allows us to visualize not only the bones, but also the discs and nerves. It shows dehydration of the discs (which appear darker), cracks in the annulus fibrosus, and detects the presence of any disc herniations or nerve compressions. In the event of contraindication to MRI, a CT scanner can be performed: it visualizes bone structures well and gives an idea of the state of the discs, but is less accurate than MRI for soft tissues.
The diagnosis of certainty is therefore based on the correlation between the symptoms of the patient, the’clinical examination and imaging results. It should be noted that there are people with signs of disc wear but no pain - you don't treat an image, you treat a patient. This is why the doctor will try to ensure that disc disease is the cause of the pain (for example, L5-S1 disc disease causing S1 sciatica). Once the diagnosis has been made, he or she can consider an appropriate treatment plan.
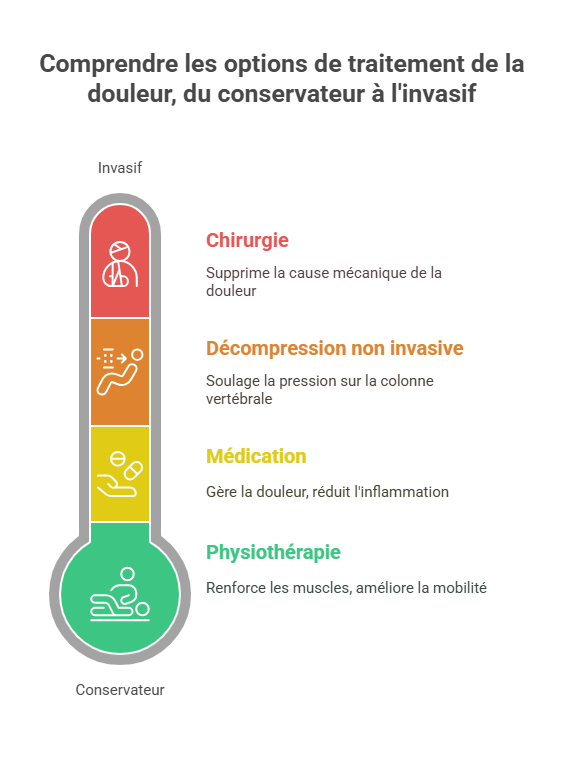
2. Available conservative treatments
Faced with a symptomatic disc degeneration, the first approach is to is curator, that is, non-surgical. The aim is to relieve pain, improve mobility and prevent worsening, without the need for immediate surgery. Several treatment options can be combined, and a personalized program will be tailored to each patient. Here are the main conservative treatments:
Medications
Various painkillers and symptomatic drugs can be prescribed, often in combination, to get through painful crises:
- Analgesics (Tier 1 or 2 painkillers: paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs) are commonly used to reduce pain and local inflammation. If pain is more intense, weak opioid analgesics (e.g. tramadol, codeine) may be used for short periods.
- Muscle relaxants (muscle relaxants): help reduce muscle spasms and contractures around the spine, which frequently occur in response to pain. Relaxing these muscles can improve mobility and reduce reflex pain. These drugs are generally prescribed overnight, as they can cause drowsiness.
- Anti-inflammatories In addition to conventional NSAIDs (ibuprofen, naproxen, etc.), short courses of oral corticosteroids (e.g. prednisone) may be considered if inflammation is very marked and radicular pain (neuralgia) persists. Corticosteroids have a powerful anti-inflammatory effect, but are only used on a short-term basis because of their side effects.
- In support, supplements of B vitamins or other adjuvants may sometimes be proposed to promote nerve health (e.g. in cases of persistent sciatica), although scientific evidence of their efficacy is limited.
It is important to note that these drugs treat symptoms (pain, stiffness) but do not «cure» the underlying disc disease. They must be used according to the doctor's instructions, in the prescribed doses and for the prescribed duration, to avoid undesirable effects (for example, NSAIDs taken long-term can irritate the stomach, and some muscle relaxants can cause drowsiness or dependence). Often, the doctor will start with paracetamol alone, then add an NSAID if necessary, and only resort to opioids or muscle relaxants if the first lines are insufficient.
Relative rest and adapted activity
In the event of an acute, very painful crisis, a period of short rest can help calm inflammation (e.g. lying down for 1-2 days if the pain is unbearable). However, this rest must be of short duration and strictly limited to the phase of intense pain. Indeed, we now know that in cases of low-back pain or neck pain caused by disc degeneration, staying in bed for too long can do more harm than good. The modern adage is« movement is the best medicine for back pain ». So, as soon as the pain allows, you should try to stay active and resume movement light. Studies have shown that a of activities encourages the recovery and prevents the onset of chronic pain. Of course, it's not a question of forcing: activities must be adapted (avoid lifting heavy objects or making strenuous movements). But walking, gentle stretching and regular movement throughout the day are encouraged, even if slight pain persists.
In practice, for example, we recommend that patients suffering from acute low back pain walk for a few minutes every hour, alternate between sitting and standing positions, and lie down temporarily if necessary, without spending the whole day in bed. Wearing a lumbar belt support can sometimes be recommended for short periods (e.g. when travelling by car, or for a specific activity) to reassure and avoid false movements, but it should not be overused to avoid further weakening the back muscles.
Physiotherapy and exercises
There physiotherapy (physical therapy in France) plays a central role in the conservative treatment of disc degeneration. A physiotherapist will be able to guide you through therapeutic exercises and manual techniques to relieve pain and strengthen the back. Common approaches include:
- Strengthening muscles The aim is to target the muscles that support the spine - in particular the paravertebral, abdominal and pelvic floor muscles. Good posture helps to stabilize the spine and reduce the load on the discs. Appropriate exercises (e.g. core strengthening exercises, modified abdominal plank, McKenzie back exercises, etc.) will be offered progressively. Strengthening improves posture and can reduce the frequency of pain.
- Stretching and mobilization The therapist may perform gentle mobilizations of the spine, stretching tense muscles (hamstrings, psoas, neck muscles, depending on the case) to improve range of motion. Manual or instrumental traction techniques can also be used to gently “unclip” vertebrae and relieve pressure on a painful disc.
- Massotherapy and heat Massage: therapeutic back massages relax contracted muscles around the painful area. Heat (hot compresses, ultrasound, etc.) can increase local blood circulation and soothe associated muscle pain.
- Postural education The physiotherapist will teach you the correct postures to adopt in everyday life to protect your back (how to bend correctly, carry an object, sit ergonomically, sleep with an adapted pillow, etc.). You'll also receive advice on how to improve your back. physical activities that respect your back will be part of the rehabilitation.
Physiotherapy often goes hand in hand with a training program.’home exercises. Your therapist will give you simple exercises to do every day at home (e.g. morning stretching exercises, light weight-bearing, regular walks) to maintain the benefits of treatment. The key is to be a player in his own recovery The more assiduous you are with your exercises and posture modifications, the better your pain will evolve over the long term. Many patients find that by continuing the exercises they learn in physio, they significantly reduce the frequency and intensity of their back pain episodes.
Infiltrations and other non-surgical procedures
If the pain remains severe despite the above measures, a specialist physician (usually a pain clinic doctor, rheumatologist or interventional radiologist) may suggest infiltrations. This involves local injections of anti-inflammatory agents (usually cortisone) close to the painful area, under radiological guidance. For example, in the case of lumbar disc degeneration with local inflammation, a corticosteroid may be injected into the epidural space or posterior joints. These infiltrations aim to reduce inflammation around the disc and nerves, providing relief that can last from a few weeks to several months. They are not systematic, but can be repeated 2-3 times a year if effective.
Other non-surgical approaches include :
- There manual spinal traction Spinal stretching: carried out by a physiotherapist or chiropractor, this involves gently stretching the spine (using an inversion table, for example, or manually) to reduce pressure on the discs. Its effects are temporary, but can provide immediate relief.
- There chiropractic Chiropractic adjustments: some patients resort to chiropractic adjustments to improve spinal mobility. Be sure to consult a qualified practitioner and inform your doctor, as not all manipulations are indicated for herniated discs.
- L’acupuncture This method of traditional Chinese medicine can help modulate pain in certain individuals and release associated muscular tension.
- There therapy neurovertebral decompression (see next section): this is a specific modality, offered in particular by TAGMED, which aims to reduce intradiscal pressure in a targeted, mechanical way. It deserves a section of its own, given its innovative nature.
In short, the conservative treatments for disc degeneration combine medication, relative rest, physiotherapy and possibly infiltrations, with the aim of improving symptoms and function. In many cases, these approaches are sufficient to control pain and enable patients to lead normal or near-normal lives, provided they adopt a healthy lifestyle to protect their backs. It's only when these measures fail or become insufficient that other, more invasive alternatives are considered.
3. Preferred treatments before considering surgery
There back surgery, Surgery, such as spinal fusion (arthrodesis) or disc replacement (disc prosthesis), is not a step to be taken lightly. As a general rule, surgery is only resorted to in the case of last resort, After all reasonable conservative options have been exhausted. In both Quebec and France, immediate surgery for degenerative disc disease is the exception rather than the rule. Indeed, the majority of patients with disc degeneration are able to relieve their symptoms through well-managed non-surgical treatments, such as those described in the previous section. Surgery is only really necessary in certain specific situations, such as :
- Persistent, incapacitating pain in spite of everything - If pain remains intense for more than 6 to 12 weeks despite optimal conservative treatment (appropriate medication, regular physio, infiltrations, etc.), and severely affects the quality of life (inability to work or function normally), then we can begin to evaluate the surgical option. Functional impact (on mobility, sleep, mood) is a major criterion.
- Progressive neurological deficit - If, in addition to pain, the associated disc disease or herniation is causing significant muscle weakness, loss of sensation or signs of nerve compression that are worsening (e.g. increasing difficulty in lifting the foot), you may need to consult your doctor. steppage - in L5 sciatica), surgery may be indicated to release the nerve before it suffers permanent damage. A warning symptom is loss of sphincter control (incontinence) or incipient ponytail syndrome, which are absolute surgical emergencies.
- Unstable structural damage - Sometimes, disc degeneration is accompanied by vertebral instability (spondylolisthesis) or progressive deformity (degenerative scoliosis). If the spine becomes unstable or excessively deformed, an operation to stabilize (fuse) the vertebrae may be necessary to prevent worsening of the condition. relieve pain mechanical instability.
Apart from these cases, degenerative disc disease is generally not considered not a serious illness in itself - it is disabling, but not fatal. Many people live with it without recourse to surgery. It's important to understand that spinal surgery, Although it relieves pain, surgery does not provide a magical “cure” for wear and tear: it treats a specific problem (a compressive hernia, an unstable movement) but does not necessarily prevent other discs from aging or vertebral joints from wearing out. Indeed, surgeons often speak of “functional” surgery for disc disease: the aim is to significantly improve the patient's situation (reduce pain, improve function), but without restoring a “young” disc or stopping the degenerative process in the other segments. This is why, even after surgery, patients must continue to take care of their backs.
Before going ahead with the operation, the doctors will make sure that all the optimal conservative treatments have been tried. This sometimes includes intensifying non-surgical management. For example:
- Meet a pain specialist to adjust medication (addition of a co-analgesic, an antineuralgic such as pregabalin if neuropathic pain, etc.).
- Follow an intensive rehabilitation in a specialized center (some clinics offer multidisciplinary programs over several weeks, with daily physio, back school, pool exercises, etc.).
- Explore alternative techniques such as neurovertebral decompression (see next section) if not already done, or other innovative modalities that may avoid surgery.
- Check that there are no modifiable external factors maintaining pain: e.g., treat an associated depressive disorder (depression can amplify pain perception), optimize sleep, adjust the workstation ergonomically, etc.
All these steps are an integral part of the “priority treatments” prior to surgery. Once we are certain that we have tried everything without success, the surgical decision can be taken more serenely, in the knowledge that it is the best remaining option for improving the patient's situation. This decision is always taken in consultation between the patient, his or her attending physician and specialist surgeon of the spine, assessing the benefit/risk balance.
In practice, if you reach this stage, the surgeon will often ask for a Recent MRI and possibly other examinations (dynamic X-rays, etc.) to help plan the procedure. He or she will explain in detail what the proposed surgery entails, what improvements can be expected, and what post-operative constraints and risks are involved. Never hesitate to ask questions - understanding the procedure is part of the informed decision-making process.
In short, surgery is considered only after less invasive solutions have been exhausted. This “cautious” approach is guided by the desire not to put the patient at unnecessary risk, and by the fact that many patients improve without a scalpel. In the following section, we will take a closer look at one of the innovative and promising conservative treatments available in Quebec: the neurovertebral decompression practiced at Clinique TAGMED.
4. TAGMED neurovertebral decompression: operation, indications and benefits
There neurovertebral decompression (DNV) is an advanced non-surgical treatment designed to treat certain back problems related to discs (herniated discs, protrusions, degenerative disc disease) and compressed nerves. It is a form of mechanically assisted and computer-controlled spinal traction. Unlike traditional traction, DNV uses sophisticated equipment - a motorized decompression table - to apply a precise traction force, modulated according to the patient and his or her pathology. Clinique TAGMED, in Quebec, is a pioneer in this approach: for over 15 years, TAGMED has distinguished itself in the field of neurovertebral decompression, earning the trust of numerous professionals. health and patients. Here's a detailed look at what this treatment is, who it's for and what the benefits are.
How does it work?
The basic principle of neurovertebral decompression is to create pressure relief within the intervertebral disc. To do this, the patient is placed comfortably on a special table, secured by harnesses (one at pelvic level, the other at torso level for the lumbar vertebrae, or a head support for the cervical vertebrae). The device then very gradually exerts tensile forces on the spine, gently pulling the vertebrae in opposite directions. A computer controls the table and adjusts traction force, angle and duration in real time, according to a precise protocol determined by the therapist. This controlled traction aims to overcome the resistance of the paravertebral muscles (which tend to contract when stretched abruptly). Thanks to the intelligent software, the machine somehow “tricks” the muscular defense reflex, enabling deep traction of the targeted vertebral segment without triggering a reflex contraction.
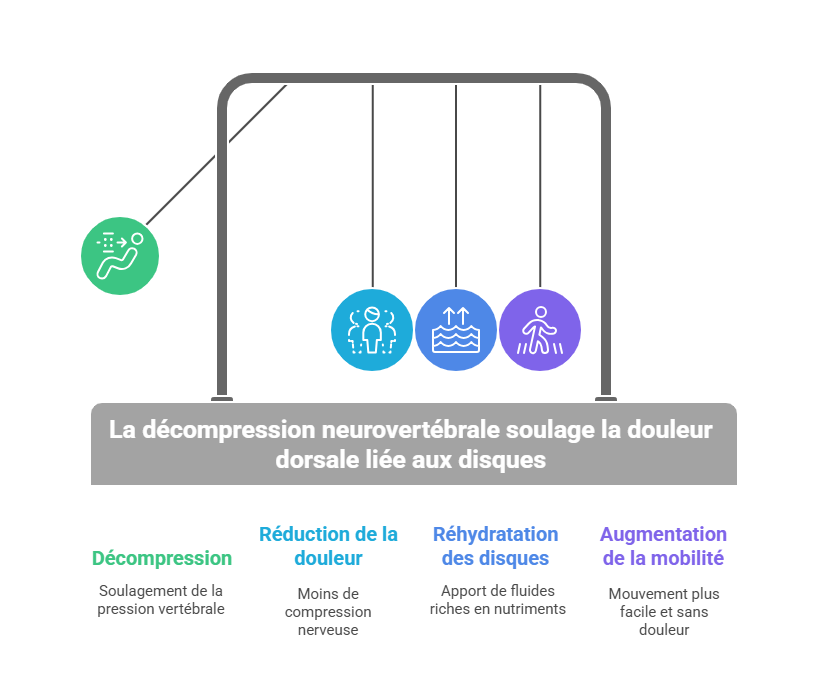
When the column is stretched in this sustained manner, a phenomenon of intradiscal negative pressure in the diseased disc. Think of the disc as a sponge: by stretching it, we create a slight vacuum inside. This negative pressure has two major effects:
- It has a suction“ force” (suction) on the disc nucleus. If part of the nucleus protrudes (herniates or protrudes), this force tends to pull it back. retract inwards of the disc. In other words, the herniated disc can gradually resorb, being “pulled” back towards the center of the disc by the pressure gradient. Imaging studies have shown that after several sessions of DNV, the herniated bulge can diminish in volume, relieving compression on the adjacent nerve.
- Negative pressure also promotes rehydration and disc regeneration. Nutrient-rich liquid is drawn into the disc (rather like a dry sponge released into water). This improved hydration can, in the medium term, improve the condition of the disc: in some cases, an increase in disc height and an improvement in disc structure have been observed after a complete decompression program. This goes hand in hand with a reduction in pain.
A typical TAGMED neurovertebral decompression session lasts approximately 30 to 45 minutes. The treatment is painless - on the contrary, many patients feel relief during traction, a sense of “letting go” from their back or neck. The protocol generally comprises several sessions (for example, 2 to 3 sessions per week for 4 to 6 weeks, depending on the condition being treated). The effect is cumulative: each session contributes a little more to decompressing the disc, healing the injury and reducing symptoms.
Illustration: Neurovertebral decompression table used at Clinique TAGMED. The patient is supported by a pelvic harness and thoracic support, while computer-controlled traction is exerted on the spine. This non-invasive procedure aims to reduce intradiscal pressure and relieve compressed nerves, offering an alternative to surgical treatment for lumbar hernias and discopathies.
Indications: for which patients and which pathologies?
Neurovertebral decompression is primarily intended for patients suffering from chronic neck or back pain related to disc pathology. Typical indications include :
- Lumbar or cervical disc herniation Hernia: whether acute or chronic, symptomatic of sciatica, cruralgia or cervicobrachial neuralgia. DNV is indicated when the hernia causes moderate nerve compression (pain, numbness) without severe neurological deficit. It can be an alternative to surgery if pain persists despite basic treatment.
- Disc protrusion (disc bulging): even without frank herniation, a degenerative disc can protrude and irritate surrounding structures. Decompression can help reduce this bulge and relieve the resulting lumbar or cervical pain.
- Isolated degenerative disc disease In the case of a patient with chronic low back pain due to a severely worn disc (black on MRI), but without a frank herniation, DNV can reduce pressure on the disc and posterior joints, providing mechanical relief.
- Moderate spinal stenosis in certain cases of narrow lumbar canal (narrowing of the canal due to osteoarthritis and ligament thickening) or of foraminal stenosis (narrowing of the nerve exit space), intermittent DNV traction can provide some relief by transiently widening the spaces and reducing nerve irritation. This does not correct the bony cause, but can relieve symptoms.
- Persistent sciatica or brachialgia When nerve-type pain persists despite medication and physio, DNV can be tried before considering epidural infiltration or surgery. It is an additional option in the therapeutic arsenal for neuralgia of disc origin.
It should be pointed out that DNV is not suitable for everyone. For example, it is not recommended in cases of spinal fusion already present on the level to be treated (since the traction would not be correct), in case of pregnancy, of vertebral fracture or’infection or tumours in the spine. It should also be avoided in patients with very severe osteoporosis or certain connective tissue diseases. Before undertaking decompression therapy, the TAGMED specialist always carefully assesses the patient's case history (clinical examination and imaging) to confirm the indication and the absence of contraindications.
Benefits and success rates
Neurovertebral decompression is an approach still considered to be of little value. innovative and is not used everywhere (in France, it's only just beginning to be known). In North America, however, many clinics have been using it for some twenty years, and studies have been published on the subject. Visit potential benefits for patients are :
- Significant reduction in pain in the lower back and neck, as well as radiating pain (legs, arms). By relieving pressure on the nerves, many patients experience a reduction in neuropathic pain (sciatica, etc.) within the first few sessions.
- Improved mobility and function Patients often report that they can resume activities they had given up because of the pain. Patients often report that they can resume activities they had given up because of the pain.
- Avoidance or postponement of surgery This is a major objective. If DNV succeeds in bringing lasting relief to a patient, this means that he or she can avoid back surgery. Even if surgery is sometimes necessary at a later date, every year gained without surgery is positive, especially in younger patients, as surgeries can be limited in number.
- Few side effects The treatment is non-invasive and very safe. The main effects may be slight muscle soreness after the first few sessions, or temporary fatigue, but compared with the effects of surgery (post-operative pain, risk of infection, etc.), these are minimal. DNV is painless during the session, and many patients even fall asleep during the treatment, which is so gentle.
Success rates vary from study to study, but overall, around 70 to 85 % of well-selected patients would derive significant benefit from neurovertebral decompression (i.e. a reduction of at least 50 % in their pain):contentReference[oaicite:2]{index=2}【3】. Of course, results depend on the severity of the pathology and the patient's commitment to the rest of the program (exercises, etc.). At Clinique TAGMED, which often combines DNV with other therapies (e.g. osteopathy, ergonomic advice, etc.), we see very good results. Several patients have testified to their relief:
«The decompression sessions eliminated my intense pain and improved my mobility. I didn't think I would ever be comfortable again, and yet it happened thanks to this treatment.» - Customer B, treated for a pinched lumbar disc
«After several sessions, I was finally able to feel better. mobility I thought lost. My back pain has diminished considerably, and I'm finally living a normal life! Of course, each case is unique and there are no absolute guarantees, but when conventional treatments have not produced the desired results, DNV represents a very interesting option to try before turning to surgery.
In short, the neurovertebral decompression offered at TAGMED is a treatment for innovative, safe and efficient for many patients suffering from disc degeneration or herniated discs. The TAGMED Clinic boasts an experienced team (over 15 years' expertise in this field) and state-of-the-art technologies. state-of-the-art to personalize treatment for each patient. The setting is clinical yet welcoming, and the staff emphasize listening and patient follow-up throughout the program. This approach is fully in line with TAGMED's philosophy of offering high-quality, non-invasive solutions to avoid surgery wherever possible, while restoring patients' optimal quality of life.
In the next section, we'll look at situations where, despite everything, surgery becomes necessary, and how these can be planned, possibly in partnership with specialist centers in France.
5. When to consider surgery in France, and why?
Despite all conservative treatments and available in Quebec (physiotherapy, medication, decompression, etc.). non-invasive at TAGMED, etc.), there are cases where the surgery becomes the most appropriate solution for relieving a patient's pain. In this section, we'll look at when you should consider surgery, why you should do it in France, and when it makes sense.
Key indications for surgery
The criteria justifying surgical intervention for degenerative disc disease or herniated discs have already been discussed (pain resistant to treatment for weeks, neurological damage, instability, etc.). In practice, a spinal surgery (such as discectomy, arthrodesis or disc prosthesis) is considered when all non-surgical measures have failed and the patient continues to suffer to such an extent that daily life is severely disrupted. For example:
- A patient who, for the past 3 months, has been unable to sleep for more than 2 hours at a stretch, can no longer walk for more than 5 minutes, has had to stop working, and has had to see a physiotherapist, drugs and infiltrations have brought little relief.
- Or a younger patient with a compressive herniated disc causing incapacitating sciatica, with the onset of loss of strength in the foot, for whom it would be risky to wait too long (or risk nerve damage).
In these situations, surgery can provide a concrete “gain”: removing the hernia compressing the nerve, stabilizing an unstable segment, freeing up a too-narrow spinal canal, etc. The aim is to remove the mechanical cause of the pain. As Dr. Queinnec pointed out functional surgeries that improve the patient's condition without rejuvenating the spine. The aim is to reduce pain and enable the patient to resume normal activities, but this does not eliminate all possibility of future back pain, nor does it stop the aging process in the other vertebrae.
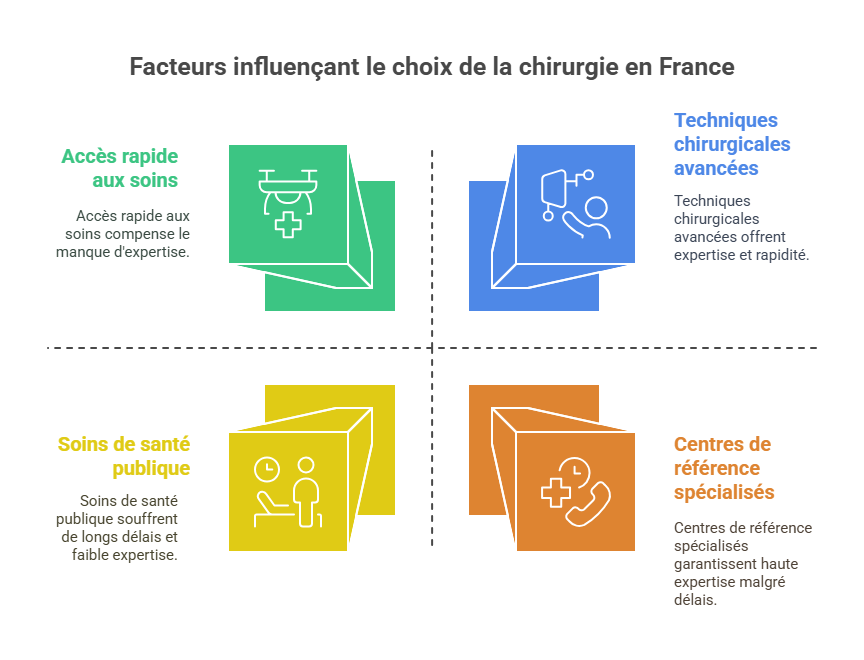
Why have surgery in France?
When surgery is necessary, the question may arise: why consider doing it in France rather than in Quebec? Here are some answers:
- Special expertise - France, and Europe in general, have been developing cutting-edge expertise in the field of spinal surgery. From techniques such as disc prosthesis (replacement of a disc by a mobile prosthesis) have been widely tested in France, whereas they are still little used in North America. Some French surgeons are internationally renowned for specific techniques (minimally invasive endoscopic surgery, robotics, 3D navigation during the operation, etc.). For example, a Quebec patient may choose France to benefit from specific expertise in a given surgical procedure. For example, the placement of disc prosthesis lumbar surgery as an alternative to fusion is relatively common in some French centers, with excellent results, which may appeal to patients wishing to maintain back mobility.
- Waiting time - Unfortunately, Quebec's public system suffers from long waiting times for non-emergency back surgery. It's not uncommon for a patient to have to wait many months, or even over a year, for an operation in a Quebec hospital, especially for “non-urgent” cases (i.e. without severe neurological deficits). This wait is painful for the suffering patient, and may prompt him or her to seek a faster alternative. In France, by opting for private management, it is often possible to obtain an operation date in just a few weeks. For someone who can no longer wait without putting their life on hold, this is a decisive factor.
- Cutting-edge reference centers - France has a number of specialized spine centers that combine high technology with high patient volumes. Establishments such as the CHU Pellegrin in Bordeaux, The Clinique du Pré in Le Mans and the Centre du Rachis in Toulouse are renowned for performing a large number of spine operations every year (over 1,000 cases/year in some centers), with state-of-the-art technical facilities including intraoperative imaging, 3D navigation, custom implants, etc. This high level of experience (case volume) is a guarantee of quality and safety. This high level of experience (case volume) is a guarantee of quality and safety: experienced surgical teams generally achieve better results and fewer complications. Quebec patients can therefore choose one of these reference centers for the assurance of a seasoned team accustomed to their specific problem.
- Support and rehabilitation - Some patients appreciate that when they travel to France for surgery, they can benefit from an on-site rehabilitation program immediately after the operation, in specialized establishments (functional rehabilitation centers). The coordination of post-operative care (physio, etc.) can sometimes be facilitated in France in a dedicated private structure, compared to a return home where the patient has to organize his own physio. It depends on the case, but it can be a factor.
- Cultural and linguistic affinities - For a French-speaking Quebecer, France is a natural choice because there is no language barrier. Communicating in one's own language with doctors, nurses and physiotherapists on site is reassuring and facilitates the care process. What's more, some of them have family in France or know the country well, which makes the stay less disorientating.
All in all, operating in France can offer rapid access to cutting-edge techniques and expert surgeons, in a French-speaking context. Of course, this has a financial cost (as it will be outside the Quebec public system), but for many patients, regaining their health is priceless. In the next section, we'll take a look at the practical organization of a surgery in France : choice of center, stay arrangements, costs and logistics.
6. Comparison of the Quebec and French approaches
It's interesting to compare the way disc degeneration and back pathologies are managed in Quebec versus France. On the whole medical principles are the same (since they are based on international scientific data), but there are differences in the way care is organized, the speed of access to certain treatments and the preferences of techniques. Here's an overview of the similarities and differences:
| In Quebec | In France |
|---|---|
|
|
In terms of care philosophy, the Quebecois and the French pursue the same goal: to relieve the patient while minimizing risks. Quebecers tend to be a little more curator (wait-and-see) approach to surgery, partly because of its system and the limited availability of back surgeons in the public sector. France will be able to offer surgery a little earlier if the criteria are met, especially since the patient can seek a second opinion more easily and even consult privately. Neither approach is “better” in itself - what's important is that the patient is at the center of decision-making and has access to the different options. What's more, we're increasingly seeing international collaboration: Quebec patients undergo surgery in France (when justified), and conversely, French experts share their know-how in Quebec via congresses or training courses.
Finally, in Quebec, the existence of clinics TAGMED, which focuses on non-invasive treatments, is an asset for patients as it fills a gap between basic physio and surgery. In France, such private decompression clinics are only just beginning to emerge (e.g. the Myodisk center in Paris). This difference shows that there is always room to learn from each other in our respective approaches.
7. Reference centers in France: Bordeaux, Le Mans, Toulouse...
If you're considering spine surgery in France, it's important to choose the right clinic or hospital. Fortunately, France has several reference centers spine surgery, with cutting-edge expertise and state-of-the-art equipment. Here's an overview of some of these centers, along with information on the surgical process, potential costs and benefits.
Bordeaux University Hospital - Centre Aquitain du Dos
Bordeaux University Hospital (Hôpital Pellegrin) is home to the Center Aquitain du Dos, a national center of excellence in spinal surgery. The team, made up of a dozen specialized surgeons, treats a wide range of degenerative lumbar and cervical pathologies (herniated discs, etc.), narrow lumbar canal, discopathy, etc.), as well as vertebral deformities (scoliosis) and traumatology. The Centre Aquitain du Dos is renowned for being at the cutting edge of minimally invasive and endoscopic techniques. For example, Dr Amélie Léglise in Bordeaux is an expert in endoscopic spinal surgery Using very small incisions (just a few millimeters) and a camera, she can remove a herniated disc or widen a narrow lumbar canal with minimal trauma to the patient:contentReference[oaicite:5]{index=5}. The benefits include reduced post-operative pain, shorter hospital stay and faster patient recovery:contentReference[oaicite:6]{index=6}. Bordeaux is also ahead of the game in performing certain surgeries in ambulatory (without spending the night in hospital) when possible - for example, they have reported cases of cervical disc prosthesis being fitted in the morning and the patient being discharged the same evening, something that is still rare elsewhere.
In terms of terms and conditions of stay, If you are having surgery in Bordeaux from abroad, you should expect to arrive a few days before the operation for preoperative consultations (anesthesia, final imaging if necessary). Hospitalization varies according to the procedure: for a simple lumbar discectomy, it's often 1 to 3 days' hospitalization; for a more extensive fusion, it can be 4-5 days. It is then advisable to stay in France for at least one or two more weeks after discharge, either in a rehabilitation center, a hotel or at an acquaintance's home, to allow time for an initial post-operative check-up with the surgeon (often 10-15 days). The Bordeaux University Hospital has an international service to help organize this. Bordeaux is also a pleasant city with good transport links (direct flights from Montreal in certain seasons, or via Paris).
In the costs In a public hospital, the cost of surgery for a non-resident includes hospital charges and surgeon's fees. These fees are generally lower than those in private clinics, but they do vary. For example, a microdiscectomy can cost several thousand euros in total. In France, prices for purely private surgery can be very high: a lumbar fusion in a private clinic can cost €15,000 to €20,000 all-in, or even more depending on the implant used. As an indication, in Germany (another reference country), a 1-level lumbar fusion costs ~29,000 € and an endoscopic nucleotomy ~13,200 €. France is in the same ballpark, though sometimes a little less expensive. It is essential to ask for a detailed estimate before confirming your surgical project. Some private international insurances may cover part of the cost if the operation is performed abroad.
Clinique du Pré - Le Mans
Located in the city of Le Mans (about 1 hour by TGV from Paris), the Clinique du Pré is a privately-owned establishment with a solid reputation in spinal surgery. Its spine unit is staffed by three experienced orthopaedic surgeons (Dr Rakover, Dr Vidal, Dr Cozma), who ensure a high quality of service. care 7 days a week and 24 hours a day in emergencies. They perform all common back operations: cervical and lumbar discectomies, multisegment arthrodeses (fusions), placement of lumbar disc prostheses, narrow lumbar canal decompression, scoliosis correction, etc. The center is particularly renowned for adult degenerative surgery, with a mastery of the latest innovations (e.g. the use of interbody fusion cages in 3D-printed peek or titanium, assisted navigation for secure screw placement, etc.). Being in a private clinic often means greater responsiveness in scheduling operations.
For an international patient, the Clinique du Pré offers a support service: their administrative department can help organize arrival, and they are used to treating patients from abroad or from other regions. Le Mans is only 1 hour by train from Paris Charles-de-Gaulle airport (direct TGV), which is a logistical plus. The post-surgery stay can be completed by a visit to the Rehabilitation center de l'Arche, also located in Le Mans, which collaborates with the clinic to care for patients after major surgery (especially for arthrodesis or scoliosis). This allows for 1 to 2 weeks of intensive rehabilitation before returning to Quebec, optimizing functional recovery.
With regard to costs, As the Clinique du Pré is a private establishment, it charges for treatment on a lump-sum basis. Personalized estimates are available on request. For example, according to some sources, a simple lumbar discectomy could cost in the region of €8,000 to €10,000 (approximately). lumbar fusion around twenty thousand euros (these figures may vary more or less depending on the case). To this must be added the cost of the rehabilitation center, if you go there. Here again, these expenses must be weighed against the cost to you of waiting longer, or the impact of not having the operation - for many, the investment is worth it if it means a quicker return to health.
Center Toulousain du Rachis - Toulouse
In Toulouse, the Center Toulousain du Rachis Sébastien Charosky and Pierre Coudert is another flagship of spinal surgery in France. Housed in the Clinique La Croix du Sud (an ultramodern facility opened in 2018), this center offers personalized care for all spinal pathology, from cervical to lumbar. Dr. Charosky is known for his expertise in complex spine surgery (he has operated on numerous scoliosis and back surgery revisions), and is at the cutting edge in terms of computer-assisted surgery and minimally invasive techniques. One of the center's highlights was its adoption of augmented reality/3D surgery: an interview on France 3 showed Dr. Charosky using a sophisticated 3D guidance system to operate with even greater precision. This illustrates the level of technology available in Toulouse.
Le centre toulousain a l’avantage d’être dans le Sud de la France, avec un climat doux et ensoleillé, ce qui n’est pas pour déplaire pendant la convalescence ! Toulouse est bien desservie (vols directs Paris-Toulouse fréquents, ou via Montréal-Paris puis TGV vers Toulouse). Pour un patient québécois, le suivi postop peut être organisé avec un contact sur place quelques semaines après, puis le relais est pris par MEDICIA ou TAGMED une fois de retour au pays en termes de suivi distant (les chirurgiens français restent joignables en cas de question).
In terms of stay, An operation in Toulouse generally involves arriving 2-3 days beforehand, a hospital stay (often between 2 and 5 days) depending on the operation, then if possible a stay in a rehabilitation center (they have reputable establishments in the Occitanie region) or a few days in a convalescent hotel. The Toulouse spine center will be able to direct you to the right resources. The secretariat, used to dealing with foreign patients, will also be able to help you with administrative formalities.
At the price list, As we are in a private clinic, we are in the same ballpark as in Le Mans. An estimate can be requested in advance. Travel costs (plane tickets, accommodation) must also be taken into account. Some clinics also offer packages including an all-inclusive package (e.g. cost of surgery + 7 days' rehab + transfers). Find out if this exists. Don't forget to keep all invoices, because even if the RAMQ doesn't reimburse non-urgent care abroad, some private insurance or tax deductions may apply.
Other centers : of course, there are other excellent centers in France - for example, the Institut Parisien du Dos (in Paris), the Clinique du Parc in Lyon, or university hospitals such as Lille and Strasbourg, which have excellent back surgery departments. neurosurgery spine. Your choice will often depend on the contact you have been recommended, or the specific technique you could benefit from. For example, for a cervical pathology, a surgeon in Paris with a reputation for cervical prostheses could be your target; for complex scoliosis, another in Lyon; and so on. The important thing is to rely on a recognized specialist. Don't hesitate to seek the advice of several surgeons if possible, to compare approaches (second opinion).
To sum up, France offers a wide range of reference centers for back surgery, combining human and technical expertise. cutting-edge technologies. Bordeaux, Le Mans and Toulouse are among the preferred options for Quebec patients, thanks to their experience and proven track record in welcoming international patients. Of course, such an overseas care project needs to be prepared in advance, often in conjunction with coordinators (TAGMED or MEDICIA, for example, can provide guidance). But for many patients, taking the step of crossing the Atlantic has been synonymous with rebirth, when they were able to undergo surgery quickly and regain a quality of life they had long since lost.
8. Patient testimonials and illustrative scenarios
To conclude this guide, there's nothing like projecting yourself through a few real-life cases of patients. We present here two fictional scenarios inspired by frequently encountered real-life situations, as well as authentic testimonials, to illustrate the care pathways and results possible. These examples are intended to reassure and demonstrate the hope that can be found in the face of painful disc degeneration.
Scenario 1: Decompression to avoid surgery (case of Mrs L.)
Profile: Mrs L. is 45 years old and works as an accountant. She has been suffering from chronic low-back pain for 2 years, due to L4-L5 and L5-S1 discopathy. An MRI scan showed two blackened discs and a small disc bulging without frank compression of the sciatic nerve. Despite physio and anti-inflammatories, the pain worsens, sometimes radiating to the right buttock. She fears she will no longer be able to do her usual activities (she likes gardening and hiking) and wants to avoid surgery.
Support : On her doctor's recommendation, Mrs L. consulted the TAGMED clinic. The osteopath interdisciplinary team confirms the indication to try the neurovertebral decompression. Un programme de 20 séances sur 6 semaines est mis en place, combiné à quelques séances d’ostéopathie pour optimiser la mobilité. Mme L. suit aussi les conseils d’exercices quotidiens que l’on lui donne (étirements du dos, renforcement abdominal).
Result: As the weeks went by, Mrs L. noticed a marked improvement. At the halfway point, she already notes a 50% reduction in her lower back pain. By the end of the sessions, she's virtually pain-free at rest, and can walk several kilometers without pain. I'm alive again! I've never virtually no back pain, I used to live with dull pain all the time. I can do a little gardening every day again. A year later, with regular maintenance of her exercises, Mrs. L. has still not needed surgery - she has resumed her activities and only has the occasional bout of moderate low back pain, which she manages with a little rest and stretching. Her case shows that»operation can be avoided using innovative conservative treatment when appropriate.
Scenario 2: Surgery in France (case of M. D.)
Profile: Mr. D. is a 52-year-old mechanic. He has a long history of back pain and was diagnosed with lumbar multistage disc disease. 6 months ago, while lifting a heavy piece of equipment, he suffered a severe sprain. herniated disc L5-S1 with paralyzing right sciatica: his right foot drags (motor deficit), and the pain is unbearable despite morphine. His life is at a standstill, and he's off work. His surgeon in Quebec recommends urgent surgery. But because of the delays, he was not operated on for another 4 months, which was unacceptable to him given the suffering.
Procedure : Through a friend, Mr. D. heard about the option of undergoing surgery in France as soon as possible. He contacted a coordinating company (MEDICIA) who organized a videoconference consultation with a spine surgeon in Bordeaux. On the basis of the MRI scan and symptoms, the surgeon confirmed the need for a L5-S1 microdiscectomy as soon as possible. Within 3 weeks, everything was planned: Mr. D. flies to France.
Surgery and follow-up : In Bordeaux, he is treated at the Centre Aquitain du Dos. The operation (removal of the hernia while preserving the disc as much as possible) took 45 minutes. The next day, he was up and walking again without sciatica - his foot gradually regaining its strength. He remains in hospital for 3 days, then spends 8 days in a rehabilitation center (balneotherapy, physio) on site. Two weeks after the operation, he was seen again by the surgeon: all was well, the scar was clean. He returned to Quebec.
Result: Two months later, Mr. D. recovered to 90%. «I felt like reborn when I woke up and the sciatic pain was gone.» His foot has regained almost all its strength. He has returned to light work (a career change was recommended to spare his back). He is very grateful to have been operated on so quickly: «If I had waited months, I might have remained disabled. Now, thanks to the team over there, I've been able to return to a normal life». Yes, disc degeneration can hurt a lot and ruin your life for a while, but today there is a wide range of treatments - from the most conservative to the most sophisticated - to help you. Many patients before you have been able to recover, avoid the wheelchair they dreaded, return to their favorite pastimes, sometimes without even needing a scalpel. For others, surgery has been a deliverance when done at the right time and by the right team. The important thing is not to give up hope, and to make sure you're well looked after medically.
Conclusion: Disc degeneration is a challenge, but with modern knowledge and collaboration between Quebec clinics (like TAGMED) and French centers, every patient can find a suitable solution. The aim of this guide is to provide you with an educational and positive overview. Feel free to consult the sources and discuss what you've read here with your healthcare professionals. You're not alone on this journey: dedicated specialists, innovative techniques and even other countries are waiting to lend you a helping hand in your quest for a better life, free from crippling pain.
Your most frequently asked questions (FAQ)
Surgical conditions
TLIF fusion is indicated for adolescent scoliosis when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Endoscopic surgery to treat herniated lumbar discs offers a modern solution with better functional results than traditional surgery.
TLIF fusion used to treat degenerative disc disease offers a modern solution with better functional results than traditional surgery.
Spondylolisthesis can be treated with fusion (e.g. TLIF, ALIF) or, in some cases, with motion-preserving devices such as TOPS™, depending on the degree of slippage and symptoms.
For patients with foraminal stenosis, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
For patients suffering from cervicarthrosic myelopathy, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Lumbar arthrodesis is indicated for vertebral fractures when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
For patients with vertebral fractures, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Treatment of degenerative disc disease in France with ALIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, vertebral fractures can be treated with Intraspine® implants, a technique renowned for its clinical results and ability to preserve spinal function.
The TLIF fusion used to treat narrow lumbar canal offers a modern solution with better functional results than traditional surgery.
The Intraspine® implant used to treat narrow lumbar spinal canal offers a modern solution with better functional results than traditional surgery.
Lumbar spinal stenosis is a narrowing of the spinal canal that compresses the nerves. In France, it can be treated by decompression surgery, sometimes accompanied by an implant such as TOPS™ or Intraspine®, to relieve pain and preserve mobility.
Treatment of vertebral fractures in France with TLIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
For patients suffering from spinal instability, the Intraspine® implant is often proposed in specialized centers due to its proven efficacy on pain and recovery.
In France, adolescent scoliosis can be treated with disc prosthesis, a technique recognized for its clinical results and ability to preserve spinal function.
In France, pseudarthrosis can be treated by endoscopic surgery, a technique recognized for its clinical results and ability to preserve spinal function.
In France, adolescent scoliosis can be treated by percutaneous surgery, a technique recognized for its clinical results and ability to preserve spinal function.
The Intraspine® implant is indicated for cervicarthrosic myelopathy when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
For patients with facet joint syndrome, endoscopic surgery is often proposed in specialized centers due to its proven efficacy on pain and recovery.
In France, pseudarthrosis can be treated by percutaneous surgery, a technique recognized for its clinical results and ability to preserve spinal function.
In France, degenerative disc disease can be treated by disc prosthesis, a technique recognized for its clinical results and ability to preserve spinal function.
In France, pseudarthrosis can be treated by endoscopic surgery, a technique recognized for its clinical results and ability to preserve spinal function.
The Intraspine® implant is indicated for cervicarthrosic myelopathy when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, pseudarthrosis can be treated by percutaneous surgery, a technique recognized for its clinical results and ability to preserve spinal function.
Disc prostheses such as LP-ESP® or CP-ESP® are used to replace a degenerative lumbar disc while maintaining spinal segment mobility.
In France, the narrow lumbar canal can be treated by endoscopic surgery, a technique recognized for its clinical results and ability to preserve spinal function.
In France, foraminal stenosis can be treated by endoscopic surgery, a technique recognized for its clinical results and ability to preserve spinal function.
Lumbar arthrodesis used to treat degenerative disc disease offers a modern solution with better functional results than traditional surgery.
Yes, the cervical disc prosthesis is an alternative to fusion that maintains neck mobility while relieving the pain caused by cervical herniation.
Lumbar arthrodesis used to treat facet joint syndrome offers a modern solution with better functional results than traditional surgery.
For patients with vertebral fractures, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
For patients with degenerative disc disease, percutaneous surgery is often proposed in specialized centers, due to its proven efficacy on pain and recovery.
In France, facet joint syndrome can be treated with Intraspine® implants, a technique renowned for its clinical results and ability to preserve spinal function.
For patients with facet joint syndrome, the TOPS™ system is often proposed in specialized centers due to its proven efficacy on pain and recovery.
For patients with facet joint syndrome, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
In France, foraminal stenosis can be treated using the TOPS™ system, a technique renowned for its clinical results and ability to preserve spinal function.
In France, kissing spine can be treated by percutaneous surgery, a technique recognized for its clinical results and ability to preserve spinal function.
Yes, several centers in France offer surgery for adult scoliosis, including multi-stage fusion techniques or endoscopic approaches to decompress the nerves.
In France, kissing spine can be treated by lumbar arthrodesis, a technique recognized for its clinical results and ability to preserve spinal function.
In France, degenerative disc disease can be treated with the TOPS™ system, a technique recognized for its clinical results and ability to preserve spinal function.
In France, ASD (Adjacent Segment Disease) can be treated by percutaneous surgery, a technique renowned for its clinical results and ability to preserve spinal function.
For patients with facet joint syndrome, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Kissing spine treatment in France by percutaneous surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, foraminal stenosis can be treated using the TOPS™ system, a technique renowned for its clinical results and ability to preserve spinal function.
The ALIF fusion used to treat narrow lumbar canal offers a modern solution with better functional results than traditional surgery.
In France, cervicarthrosic myelopathy can be treated by lumbar arthrodesis, a technique recognized for its clinical results and ability to preserve spinal function.
The TOPS™ system is indicated for vertebral fractures when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
The TLIF fusion used to treat ASD (Adjacent Segment Disease) offers a modern solution with better functional results than traditional surgery.
The Intraspine® implant is indicated for degenerative disc disease when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Treatment of degenerative disc disease in France with Intraspine® implants is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Spondylolisthesis can be treated with fusion (e.g. TLIF, ALIF) or, in some cases, with motion-preserving devices such as TOPS™, depending on the degree of slippage and symptoms.
For patients suffering from cervicarthrosic myelopathy, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
For patients with vertebral fractures, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Disc prosthesis is indicated for degenerative disc disease when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, facet joint syndrome can be treated by endoscopic surgery, a technique renowned for its clinical results and ability to preserve spinal function.
ALIF fusion is indicated for adolescent scoliosis when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
The TOPS™ system used to treat ASD (Adjacent Segment Disease) offers a modern solution with better functional results compared to traditional surgery.
For patients with foraminal stenosis, percutaneous surgery is often proposed in specialized centers, due to its proven efficacy on pain and recovery.
In France, kissing spine can be treated by percutaneous surgery, a technique recognized for its clinical results and ability to preserve spinal function.
TLIF fusion used to treat degenerative disc disease offers a modern solution with better functional results than traditional surgery.
Kissing spine treatment in France with disc prosthesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Treatment of narrow lumbar spinal canal in France by percutaneous surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Treatment of lumbar disc herniation in France by lumbar arthrodesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Yes, the cervical disc prosthesis is an alternative to fusion that maintains neck mobility while relieving the pain caused by cervical herniation.
For patients with vertebral fractures, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
In France, facet joint syndrome can be treated with Intraspine® implants, a technique renowned for its clinical results and ability to preserve spinal function.
Treatment of degenerative disc disease in France with TLIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The TLIF fusion used to treat ASD (Adjacent Segment Disease) offers a modern solution with better functional results than traditional surgery.
The treatment of ASD (Adjacent Segment Disease) in France with Intraspine® implants is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The Intraspine® implant is indicated for degenerative disc disease when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Treatment of spinal instability in France with TLIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Treatment of degenerative disc disease in France with Intraspine® implants is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, adolescent scoliosis can be treated with disc prosthesis, a technique recognized for its clinical results and ability to preserve spinal function.
The disc prosthesis used to treat kissing spine offers a modern solution with better functional results than traditional surgery.
Endoscopic surgery is indicated for ASD (Adjacent Segment Disease) when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, vertebral fractures can be treated with ALIF fusion, a technique renowned for its clinical results and ability to preserve spinal function.
In France, facet joint syndrome can be treated by endoscopic surgery, a technique renowned for its clinical results and ability to preserve spinal function.
The TOPS™ system used to treat ASD (Adjacent Segment Disease) offers a modern solution with better functional results compared to traditional surgery.
In France, cervicarthrosic myelopathy can be treated by lumbar arthrodesis, a technique recognized for its clinical results and ability to preserve spinal function.
For patients with cervicarthrosic myelopathy, percutaneous surgery is often proposed in specialized centers, due to its proven efficacy on pain and recovery.
ALIF fusion is indicated for kissing spine when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
The Intraspine® implant is indicated for vertebral fractures when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Disc prosthesis is indicated for facet joint syndrome when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, cervicarthrosic myelopathy can be treated by disc prosthesis, a technique recognized for its clinical results and ability to preserve spinal function.
In France, facet joint syndrome can be treated using the TOPS™ system, a technique renowned for its clinical results and ability to preserve spinal function.
Lumbar arthrodesis used to treat degenerative disc disease offers a modern solution with better functional results than traditional surgery.
Percutaneous surgery to treat narrow lumbar spinal canal offers a modern solution with better functional results than traditional surgery.
Endoscopic surgery to treat spinal instability offers a modern solution with better functional results than traditional surgery.
Lumbar arthrodesis used to treat lumbar disc herniation offers a modern solution with better functional results than traditional surgery.
ALIF fusion is indicated for kissing spine when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Disc prosthesis is indicated for facet joint syndrome when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, facet joint syndrome can be treated using the TOPS™ system, a technique renowned for its clinical results and ability to preserve spinal function.
Treatment of pseudarthrosis in France with the TOPS™ system is part of a structured pathway with initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The treatment of spinal instability in France with Intraspine® implants is part of a structured approach involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Treatment of facet joint syndrome in France by lumbar arthrodesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The ALIF fusion used to treat cervicarthrosis myelopathy offers a modern solution with better functional results than traditional surgery.
Percutaneous surgery to treat herniated lumbar discs offers a modern solution with better functional results than traditional surgery.
Treatment of lumbar disc herniation in France by lumbar arthrodesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, ASD (Adjacent Segment Disease) can be treated by percutaneous surgery, a technique renowned for its clinical results and ability to preserve spinal function.
In France, the narrow lumbar canal can be treated with TLIF fusion, a technique renowned for its clinical results and ability to preserve spinal function.
In France, kissing spine can be treated with TLIF fusion, a technique renowned for its clinical results and ability to preserve spinal function.
The treatment of pseudarthrosis in France by endoscopic surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The treatment of spinal instability in France with Intraspine® implants is part of a structured approach involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The ALIF fusion used to treat cervicarthrosis myelopathy offers a modern solution with better functional results than traditional surgery.
TLIF fusion is indicated for cervicarthrosis myelopathy when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Kissing spine treatment in France by endoscopic surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Kissing spine treatment in France with disc prosthesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
TLIF fusion is indicated for adolescent scoliosis when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Treatment of narrow lumbar spinal canal in France by percutaneous surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Endoscopic surgery to treat herniated lumbar discs offers a modern solution with better functional results than traditional surgery.
TLIF fusion is indicated for cervicarthrosis myelopathy when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Disc prosthesis is indicated for degenerative disc disease when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, kissing spine can be treated by endoscopic surgery, a technique recognized for its clinical results and ability to preserve spinal function.
Endoscopic surgery to treat adolescent scoliosis offers a modern solution with better functional results than traditional surgery.
Lumbar arthrodesis used to treat pseudarthrosis offers a modern solution with better functional results than traditional surgery.
The treatment of adolescent scoliosis in France by endoscopic surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The TOPS™ system used to treat narrow lumbar canal offers a modern solution with better functional results compared to traditional surgery.
In France, foraminal stenosis can be treated with ALIF fusion, a technique renowned for its clinical results and ability to preserve spinal function.
In France, narrow lumbar spinal canal can be treated by lumbar arthrodesis, a technique recognized for its clinical results and ability to preserve spinal function.
The disc prosthesis used to treat kissing spine offers a modern solution with better functional results than traditional surgery.
For patients with ASD (Adjacent Segment Disease), lumbar arthrodesis is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Endoscopic surgery is indicated for ASD (Adjacent Segment Disease) when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
For patients suffering from spinal instability, endoscopic surgery is often proposed in specialized centers due to its proven efficacy on pain and recovery.
In France, vertebral fractures can be treated with ALIF fusion, a technique renowned for its clinical results and ability to preserve spinal function.
Treatment of degenerative disc disease in France with TLIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, adolescent scoliosis can be treated by percutaneous surgery, a technique recognized for its clinical results and ability to preserve spinal function.
For patients with facet joint syndrome, endoscopic surgery is often proposed in specialized centers due to its proven efficacy on pain and recovery.
The TOPS™ system used to treat adolescent scoliosis offers a modern solution with better functional results compared to traditional surgery.
Treatment of narrow lumbar spinal canal in France with disc prosthesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
TLIF fusion is indicated for kissing spine when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Lumbar spinal stenosis is a narrowing of the spinal canal that compresses the nerves. In France, it can be treated by decompression surgery, sometimes accompanied by an implant such as TOPS™ or Intraspine®, to relieve pain and preserve mobility.
The treatment of adolescent scoliosis in France by endoscopic surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Treatment of vertebral fractures in France with TLIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The TOPS™ system used to treat narrow lumbar canal offers a modern solution with better functional results compared to traditional surgery.
For patients suffering from spinal instability, the Intraspine® implant is often proposed in specialized centers due to its proven efficacy on pain and recovery.
In France, foraminal stenosis can be treated with ALIF fusion, a technique renowned for its clinical results and ability to preserve spinal function.
For patients with cervicarthrosic myelopathy, percutaneous surgery is often proposed in specialized centers, due to its proven efficacy on pain and recovery.
Kissing spine treatment in France by percutaneous surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The ALIF fusion used to treat narrow lumbar canal offers a modern solution with better functional results than traditional surgery.
The TLIF fusion used to treat pseudarthrosis offers a modern solution with better functional results than traditional surgery.
Endoscopic surgery is indicated for facet joint syndrome when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Treatment of facet joint syndrome in France with disc prosthesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, vertebral fractures can be treated by lumbar arthrodesis, a technique renowned for its clinical results and ability to preserve spinal function.
Percutaneous surgery to treat narrow lumbar spinal canal offers a modern solution with better functional results than traditional surgery.
Treatment of pseudarthrosis in France with TLIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Endoscopic surgery to treat spinal instability offers a modern solution with better functional results than traditional surgery.
For patients with spinal instability, TLIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Lumbar arthrodesis used to treat lumbar disc herniation offers a modern solution with better functional results than traditional surgery.
Treatment of pseudarthrosis in France with the TOPS™ system is part of a structured pathway with initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The treatment of ASD (Adjacent Segment Disease) in France with Intraspine® implants is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Treatment of spinal instability in France with TLIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
For patients with foraminal stenosis, ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Lumbar arthrodesis is indicated for vertebral fractures when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Treatment of degenerative disc disease in France with ALIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Disc prostheses such as LP-ESP® or CP-ESP® are used to replace a degenerative lumbar disc while maintaining spinal segment mobility.
The TOPS™ system used to treat adolescent scoliosis offers a modern solution with better functional results compared to traditional surgery.
In France, the narrow lumbar canal can be treated by endoscopic surgery, a technique recognized for its clinical results and ability to preserve spinal function.
Treatment of narrow lumbar spinal canal in France with disc prosthesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, foraminal stenosis can be treated by endoscopic surgery, a technique recognized for its clinical results and ability to preserve spinal function.
TLIF fusion is indicated for kissing spine when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
Kissing spine treatment in France by endoscopic surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Treatment of facet joint syndrome in France by lumbar arthrodesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
Percutaneous surgery to treat herniated lumbar discs offers a modern solution with better functional results than traditional surgery.
Lumbar arthrodesis used to treat facet joint syndrome offers a modern solution with better functional results than traditional surgery.
For patients with degenerative disc disease, percutaneous surgery is often proposed in specialized centers, due to its proven efficacy on pain and recovery.
In France, degenerative disc disease can be treated by disc prosthesis, a technique recognized for its clinical results and ability to preserve spinal function.
The treatment of pseudarthrosis in France by endoscopic surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, the narrow lumbar canal can be treated with TLIF fusion, a technique renowned for its clinical results and ability to preserve spinal function.
The TLIF fusion used to treat pseudarthrosis offers a modern solution with better functional results than traditional surgery.
In France, kissing spine can be treated with TLIF fusion, a technique renowned for its clinical results and ability to preserve spinal function.
For patients with ASD (Adjacent Segment Disease), ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
The treatment of pseudarthrosis in France by endoscopic surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, narrow lumbar spinal canal can be treated by lumbar arthrodesis, a technique recognized for its clinical results and ability to preserve spinal function.
For patients with ASD (Adjacent Segment Disease), lumbar arthrodesis is often proposed in specialized centers due to its proven efficacy on pain and recovery.
For patients suffering from spinal instability, endoscopic surgery is often proposed in specialized centers due to its proven efficacy on pain and recovery.
ALIF fusion is indicated for adolescent scoliosis when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
For patients with foraminal stenosis, percutaneous surgery is often proposed in specialized centers, due to its proven efficacy on pain and recovery.
For patients with facet joint syndrome, the TOPS™ system is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Yes, several centers in France offer surgery for adult scoliosis, including multi-stage fusion techniques or endoscopic approaches to decompress the nerves.
The TLIF fusion used to treat pseudarthrosis offers a modern solution with better functional results than traditional surgery.
In France, kissing spine can be treated by lumbar arthrodesis, a technique recognized for its clinical results and ability to preserve spinal function.
Endoscopic surgery is indicated for facet joint syndrome when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, degenerative disc disease can be treated with the TOPS™ system, a technique recognized for its clinical results and ability to preserve spinal function.
Treatment of facet joint syndrome in France with disc prosthesis is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
In France, vertebral fractures can be treated by lumbar arthrodesis, a technique renowned for its clinical results and ability to preserve spinal function.
Treatment of pseudarthrosis in France with TLIF fusion is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
For patients with spinal instability, TLIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
The Intraspine® implant is indicated for vertebral fractures when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, cervicarthrosic myelopathy can be treated by disc prosthesis, a technique recognized for its clinical results and ability to preserve spinal function.
The TOPS™ system is indicated for vertebral fractures when conservative treatment has failed. It provides effective relief while reducing the risk of post-operative complications.
In France, vertebral fractures can be treated with Intraspine® implants, a technique renowned for its clinical results and ability to preserve spinal function.
In France, kissing spine can be treated by endoscopic surgery, a technique recognized for its clinical results and ability to preserve spinal function.
The TLIF fusion used to treat narrow lumbar canal offers a modern solution with better functional results than traditional surgery.
Endoscopic surgery to treat adolescent scoliosis offers a modern solution with better functional results than traditional surgery.
The Intraspine® implant used to treat narrow lumbar spinal canal offers a modern solution with better functional results than traditional surgery.
Lumbar arthrodesis used to treat pseudarthrosis offers a modern solution with better functional results than traditional surgery.
The treatment of pseudarthrosis in France by endoscopic surgery is part of a structured pathway involving initial assessment, minimally invasive surgery and personalized post-operative follow-up.
The TLIF fusion used to treat pseudarthrosis offers a modern solution with better functional results than traditional surgery.
For patients with ASD (Adjacent Segment Disease), ALIF fusion is often proposed in specialized centers due to its proven efficacy on pain and recovery.
Your most frequently asked questions (FAQ)
Disc degeneration
Thanks to a targeted approach, B-Dyn® dynamic implant treatment effectively treats the black disc on MRI by intervening on the mechanical cause of the problem.
If segmental disc instability does not respond to non-surgical treatments, disc prosthesis becomes an option for restoring stability and comfort.
If disc degeneration with chronic pain does not respond to non-surgical treatments, arthrodesis with interbody cage becomes an option to restore stability and comfort.
In the case of multisegmental disc degeneration, dynamic treatment with B-Dyn® implants either replaces the disc or stabilizes the affected segment to reduce mechanical pain.
Thanks to a targeted approach, minimally invasive disc recalibration surgery effectively treats symptomatic disc height loss by addressing the mechanical cause of the problem.
In the case of symptomatic disc height loss, dynamic treatment with B-Dyn® implants either replaces the disc or stabilizes the affected segment to reduce mechanical pain.
Thanks to a targeted approach, minimally invasive disc recalibration surgery effectively treats disc degeneration with chronic pain by intervening on the mechanical cause of the problem.
In patients with black disc on MRI, dynamic treatment with B-Dyn® implants can significantly improve mobility, reduce pain and limit degenerative progression.
In the case of degenerative disc disease, dynamic treatment with B-Dyn® implants either replaces the disc or stabilizes the affected segment to reduce mechanical pain.
Thanks to a targeted approach, minimally invasive disc recalibration surgery effectively treats segmental disc instability by intervening on the mechanical cause of the problem.
If the black disc on MRI does not respond to non-surgical treatment, arthrodesis with interbody cage becomes an option to restore stability and comfort.
Thanks to a targeted approach, disc prosthesis effectively treats intervertebral disc wear by intervening on the mechanical cause of the problem.
In the case of segmental disc instability, disc prosthesis either replaces the disc or stabilizes the affected segment to reduce mechanical pain.
If multisegmental disc degeneration does not respond to non-surgical treatments, arthrodesis with interbody cage becomes an option for restoring stability and comfort.
In patients with degenerative disc disease, disc prosthesis can significantly improve mobility, reduce pain and limit degenerative progression.
In patients with black disc on MRI, lumbar fusion can significantly improve mobility, reduce pain and limit degenerative progression.
Dynamic treatment with B-Dyn® implants is indicated to relieve the pain associated with symptomatic loss of disc height, when the disc no longer plays its role as a shock absorber.
Lumbar fusion is indicated to relieve pain associated with disc degeneration and chronic pain when the disc no longer plays its role as a shock absorber.
In the event of intervertebral disc wear, arthrodesis with an interbody cage can either replace the disc, or stabilize the affected segment to reduce mechanical pain.
Disc prosthesis is indicated to relieve pain associated with a black disc on MRI, when the disc no longer plays its role as a shock absorber.
In cases of symptomatic disc height loss, lumbar fusion can either replace the disc or stabilize the affected segment to reduce mechanical pain.
In the case of multisegmental disc degeneration, minimally invasive disc recalibration surgery can either replace the disc or stabilize the affected segment to reduce mechanical pain.
Thanks to a targeted approach, disc prosthesis effectively treats the black disc on MRI by intervening on the mechanical cause of the problem.
In patients with MRI-black discs, minimally invasive disc recalibration surgery can significantly improve mobility, reduce pain and limit degenerative progression.
In patients with intervertebral disc wear, dynamic treatment with B-Dyn® implants can significantly improve mobility, reduce pain and limit degenerative progression.
Thanks to its targeted approach, arthrodesis with interbody cage effectively treats degenerative disc disease by addressing the mechanical cause of the problem.
Arthrodesis with interbody cage is indicated to relieve pain associated with segmental disc instability when the disc no longer plays its role as a shock absorber.
Thanks to a targeted approach, B-Dyn® dynamic implant therapy effectively treats disc degeneration with chronic pain by addressing the mechanical cause of the problem.
In cases of symptomatic disc height loss, targeted endoscopic surgery can either replace the disc or stabilize the affected segment to reduce mechanical pain.
In cases of degenerative disc disease, targeted endoscopic surgery can either replace the disc or stabilize the affected segment to reduce mechanical pain.
If intervertebral disc wear does not respond to non-surgical treatment, lumbar fusion becomes an option for restoring stability and comfort.
Minimally invasive disc recalibration surgery is indicated to relieve pain associated with disc degeneration with chronic pain when the disc no longer plays its role as a shock absorber.
In patients with black disc on MRI, arthrodesis with interbody cage can significantly improve mobility, reduce pain and limit degenerative progression.
Lumbar fusion is indicated to relieve pain associated with a black disc on MRI, when the disc no longer plays its role as a shock absorber.
In patients with intervertebral disc wear, arthrodesis with an interbody cage can significantly improve mobility, reduce pain and limit degenerative progression.
Disc prosthesis is indicated to relieve pain associated with segmental disc instability, when the disc no longer plays its role as a shock absorber.
In patients with symptomatic disc height loss, dynamic treatment with B-Dyn® implants can significantly improve mobility, reduce pain and limit degenerative progression.
In patients with multisegmental disc degeneration, disc prosthesis can significantly improve mobility, reduce pain and limit degenerative progression.
Thanks to a targeted approach, targeted endoscopic surgery effectively treats multisegmental disc degeneration by intervening on the mechanical cause of the problem.
If degenerative disc disease does not respond to non-surgical treatments, minimally invasive disc recalibration surgery becomes an option for restoring stability and comfort.
In patients with multisegmental disc degeneration, dynamic treatment with B-Dyn® implants can significantly improve mobility, reduce pain and limit degenerative progression.
In the case of degenerative disc disease, minimally invasive disc recalibration surgery can either replace the disc or stabilize the affected segment to reduce mechanical pain.
Thanks to a targeted approach, minimally invasive disc recalibration surgery effectively treats symptomatic disc height loss by addressing the mechanical cause of the problem.
Minimally invasive disc recalibration surgery is indicated to relieve pain associated with disc degeneration with chronic pain when the disc no longer plays its role as a shock absorber.
If symptomatic disc height loss does not respond to non-surgical treatments, arthrodesis with interbody cage becomes an option for restoring stability and comfort.
Thanks to a targeted approach, disc prosthesis effectively treats intervertebral disc wear by intervening on the mechanical cause of the problem.
Disc prosthesis is indicated to relieve the pain associated with degenerative disc disease, when the disc no longer plays its role as a shock absorber.
In the case of degenerative disc disease, minimally invasive disc recalibration surgery can either replace the disc or stabilize the affected segment to reduce mechanical pain.
Minimally invasive disc recalibration surgery is indicated to relieve pain associated with segmental disc instability when the disc no longer plays its role as a shock absorber.
Thanks to a targeted approach, disc prosthesis effectively treats segmental disc instability by acting on the mechanical cause of the problem.
In patients with degenerative disc disease, targeted endoscopic surgery can significantly improve mobility, reduce pain and limit degenerative progression.
Thanks to a targeted approach, B-Dyn® dynamic implant therapy effectively treats degenerative disc disease by addressing the mechanical cause of the problem.
If the black disc on MRI does not respond to non-surgical treatment, lumbar fusion becomes an option to restore stability and comfort.
In the case of multisegmental disc degeneration, disc prosthesis can either replace the disc or stabilize the affected segment to reduce mechanical pain.
Thanks to a targeted approach, targeted endoscopic surgery effectively treats disc degeneration with chronic pain by intervening on the mechanical cause of the problem.
In patients with segmental disc instability, lumbar fusion can significantly improve mobility, reduce pain and limit degenerative progression.
Thanks to a targeted approach, minimally invasive disc recalibration surgery effectively treats degenerative disc disease by intervening on the mechanical cause of the problem.
Thanks to a targeted approach, disc prosthesis effectively treats multisegmental disc degeneration by acting on the mechanical cause of the problem.
If disc degeneration with chronic pain does not respond to non-surgical treatments, targeted endoscopic surgery becomes an option for restoring stability and comfort.
In the event of intervertebral disc wear, dynamic treatment with B-Dyn® implants either replaces the disc or stabilizes the affected segment to reduce mechanical pain.
Lumbar fusion is indicated to relieve pain associated with disc degeneration and chronic pain when the disc no longer plays its role as a shock absorber.
If disc degeneration with chronic pain does not respond to non-surgical treatments, lumbar fusion becomes an option for restoring stability and comfort.
In patients with symptomatic disc height loss, targeted endoscopic surgery can significantly improve mobility, reduce pain and limit degenerative progression.
In the event of intervertebral disc wear, targeted endoscopic surgery can either replace the disc or stabilize the affected segment to reduce mechanical pain.
In patients with symptomatic disc height loss, arthrodesis with interbody cage can significantly improve mobility, reduce pain and limit degenerative progression.
Thanks to a targeted approach, lumbar fusion effectively treats the black disc on MRI by intervening on the mechanical cause of the problem.
In the case of symptomatic disc height loss, disc prosthesis can either replace the disc or stabilize the affected segment to reduce mechanical pain.
Disc prosthesis is indicated to relieve pain associated with a black disc on MRI, when the disc no longer plays its role as a shock absorber.
Arthrodesis with interbody cage is indicated to relieve pain associated with segmental disc instability when the disc no longer plays its role as a shock absorber.
Minimally invasive disc recalibration surgery is indicated to relieve pain associated with symptomatic loss of disc height, when the disc no longer plays its role as a shock absorber.
In patients with segmental disc instability, minimally invasive disc recalibration surgery can significantly improve mobility, reduce pain and limit degenerative progression.
If the black disc on MRI does not respond to non-surgical treatment, arthrodesis with interbody cage becomes an option to restore stability and comfort.
Thanks to a targeted approach, B-Dyn® dynamic implant therapy effectively treats disc degeneration with chronic pain by addressing the mechanical cause of the problem.
Thanks to a targeted approach, disc prosthesis effectively treats symptomatic disc height loss by addressing the mechanical cause of the problem.
If intervertebral disc wear does not respond to non-surgical treatments, arthrodesis with interbody cage becomes an option to restore stability and comfort.
In patients with intervertebral disc wear, disc prosthesis can considerably improve mobility, reduce pain and limit degenerative progression.
In patients with MRI-black discs, disc prosthesis can significantly improve mobility, reduce pain and limit degenerative progression.
If segmental disc instability does not respond to non-surgical treatment, arthrodesis with interbody cage becomes an option for restoring stability and comfort.
If multisegmental disc degeneration does not respond to non-surgical treatments, lumbar fusion becomes an option for restoring stability and comfort.
Thanks to a targeted approach, arthrodesis with interbody cage effectively treats multisegmental disc degeneration by intervening on the mechanical cause of the problem.
In the case of multisegmental disc degeneration, lumbar fusion can either replace the disc or stabilize the affected segment to reduce mechanical pain.
If multisegmental disc degeneration does not respond to non-surgical treatments, targeted endoscopic surgery becomes an option for restoring stability and comfort.
Arthrodesis with interbody cage is indicated to relieve pain related to disc degeneration with chronic pain when the disc no longer plays its role as a shock absorber.
Thanks to its targeted approach, B-Dyn® dynamic implant therapy effectively treats symptomatic disc height loss by addressing the mechanical cause of the problem.
In patients with chronically painful disc degeneration, arthrodesis with an interbody cage can significantly improve mobility, reduce pain and limit degenerative progression.
Minimally invasive disc recalibration surgery is indicated to relieve pain associated with symptomatic loss of disc height, when the disc no longer plays its role as a shock absorber.
Minimally invasive disc recalibration surgery is indicated to relieve pain associated with a black disc on MRI when the disc no longer plays its role as a shock absorber.
Thanks to a targeted approach, minimally invasive disc recalibration surgery effectively treats degenerative disc disease by intervening on the mechanical cause of the problem.
If intervertebral disc wear does not respond to non-surgical treatments, minimally invasive disc recalibration surgery becomes an option for restoring stability and comfort.
In cases of symptomatic disc height loss, minimally invasive disc recalibration surgery can either replace the disc or stabilize the affected segment to reduce mechanical pain.
In the event of a black disc on MRI, lumbar fusion can either replace the disc or stabilize the affected segment to reduce mechanical pain.
In patients with intervertebral disc wear, dynamic treatment with B-Dyn® implants can significantly improve mobility, reduce pain and limit degenerative progression.
If degenerative disc disease does not respond to non-surgical treatments, dynamic treatment with B-Dyn® implants becomes an option for restoring stability and comfort.
If disc degeneration with chronic pain does not respond to non-surgical treatments, lumbar fusion becomes an option for restoring stability and comfort.